The Impact of Oral Bacteria on Overall Health
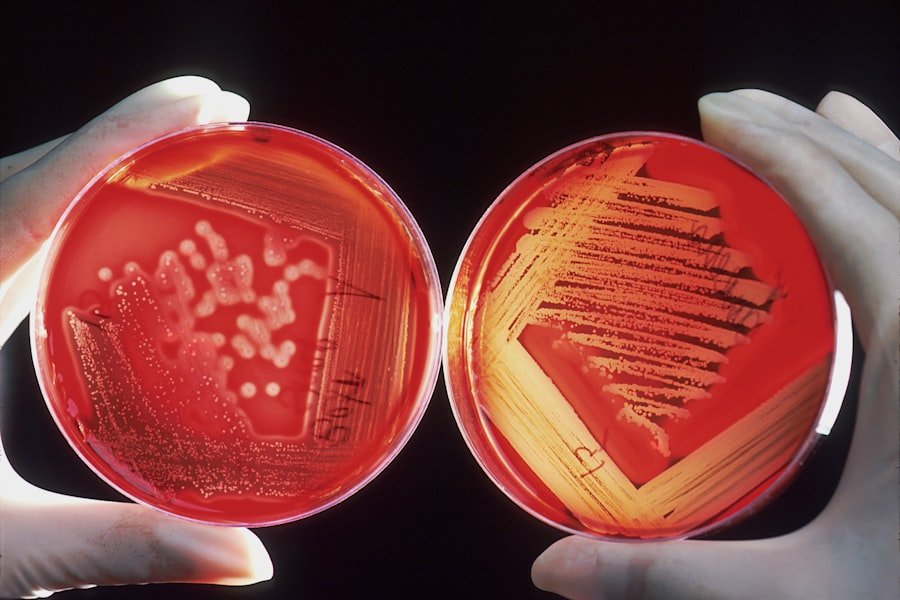
We often consider our mouths as a mere gateway for food and speech, a functional apparatus operating somewhat independently of the rest of our bodies. However, this perspective is a profound oversight. Our oral cavity, far from being an isolated system, is a bustling metropolis of microbial life, a complex ecosystem where trillions of bacteria meticulously interact with one another and with our host tissues. This intricate community, known as the oral microbiome, holds a surprisingly powerful sway over our overall health. We are only now, through the relentless pursuit of scientific understanding, beginning to fully appreciate the profound and often invisible connections between our oral bacteria and systemic well-being. This article will explore these critical links, delving into how the microscopic residents of our mouths can be both guardians and saboteurs of our health.
Within the warm, moist confines of our mouths, a diverse array of bacteria, fungi, viruses, and archaea thrive, forming a dynamic and adaptable community. This ecosystem is not static; it constantly adapts to our dietary choices, hygiene practices, and even our stress levels. A [dental abscess](https://youtu.be/3ZdKOXDCyt4?si=QVBTEqo_RpxW7c4T) is a painful infection at the root of a tooth or between the gum and a tooth.
A Balancing Act: Commensals and Pathogens
We maintain a delicate balance within our oral microbiome. Commensal bacteria, the “good” guys, outnumber the “bad” guys (potential pathogens) in a healthy mouth. These beneficial microbes play a crucial role in maintaining oral homeostasis. They compete with harmful bacteria for resources and attachment sites, deterring their unchecked proliferation. They can also contribute to nutrient metabolism and even support local immune responses. Conversely, when this equilibrium is disrupted, say by poor oral hygiene or a sugar-rich diet, opportunistic pathogens can gain a foothold. This shift in the microbial landscape, known as dysbiosis, is the cornerstone of many oral and systemic diseases. Imagine it as a bustling city where law-abiding citizens (commensals) keep the peace, but a sudden influx of a criminal element (pathogens) can quickly lead to societal breakdown.
Biofilms: The Microbial Cities
Oral bacteria don’t just float around individually; they organize themselves into highly structured communities called biofilms. Dental plaque, the sticky film we feel on our teeth, is a prime example of a biofilm. These matrix-embedded communities offer a protective environment for bacteria, shielding them from antimicrobial agents and host immune defenses. The architecture of biofilms allows for intricate intercellular communication and nutrient cycling, making them remarkably resilient. It’s like a well-fortified city wall, protecting its inhabitants from external threats and allowing for efficient internal resource management.
Recent studies have highlighted the significant role that oral bacteria play in overall health, linking them to various systemic conditions. For a deeper understanding of this connection, you can explore the article that discusses the implications of oral microbiota on human health. To read more about this topic, visit this article.
Oral Diseases Spanning Beyond the Mouth
The most direct and widely recognized impact of oral bacteria is on the health of our teeth and gums. These localized infections, often dismissed as mere nuisances, are in fact significant indicators of underlying dysbiosis and can act as springboards for broader health issues.
Dental Caries: The Erosion of Enamel
Dental caries, commonly known as tooth decay or cavities, remains one of the most prevalent chronic diseases globally. It is primarily caused by specific acid-producing bacteria, predominantly Streptococcus mutans and Lactobacillus species. These bacteria metabolize dietary sugars, producing lactic acid that demineralizes the tooth enamel. Over time, persistent acid attacks lead to the formation of cavities. We understand that a diet high in fermentable carbohydrates feeds these acid-producing bacteria, allowing them to flourish and tilt the microbial balance towards destruction. This is a classic example of how our lifestyle choices directly fuel the destructive tendencies of specific oral microbes.
Periodontal Disease: The Silent Destroyer
Periodontal disease, or gum disease, encompasses a spectrum of inflammatory conditions affecting the tissues surrounding and supporting our teeth. It begins as gingivitis, a reversible inflammation of the gums, characterized by redness, swelling, and bleeding. If left untreated, gingivitis can progress to periodontitis, a more severe and irreversible form characterized by bone loss supporting the teeth. Specific anaerobic bacteria, such as Porphyromonas gingivalis, Tannerella forsythia, and Treponema denticola, are strongly implicated in the pathogenesis of periodontitis. These pathogens trigger a chronic inflammatory response that, while initially aimed at eliminating the bacteria, ultimately damages the host tissues, leading to tooth loosening and eventual tooth loss. Imagine a low-grade war festering in the tissues surrounding the teeth, where the initial defensive response becomes a destructive force within itself.
The Systemic Reach: Connecting Oral Health to Cardiovascular Disease

One of the most compelling and intensively researched connections between oral bacteria and systemic health lies in their relationship with cardiovascular diseases (CVDs), particularly atherosclerosis. We are increasingly recognizing the oral cavity not as a separate entity, but as an integral part of the vascular network.
The Inflammation Highway: From Gums to Arteries
The chronic inflammation characteristic of periodontitis doesn’t just stay confined to the gums. The inflammatory mediators produced in response to periodontal pathogens, such as cytokines and C-reactive protein (CRP), can enter the bloodstream. These circulating inflammatory molecules contribute to systemic inflammation, a known risk factor for atherosclerosis. It’s akin to a brushfire in one part of a forest sending embers flying, igniting smaller fires elsewhere.
Direct Invasion: Bacteria in the Bloodstream
Periodontal pathogens themselves can directly enter the bloodstream, a phenomenon known as bacteremia, which often occurs during routine activities like chewing or brushing, especially in individuals with compromised gum tissue. Once in the circulation, these bacteria or their components, such as lipopolysaccharides (LPS), can adhere to the walls of blood vessels. Studies have detected periodontal bacteria, including Porphyromonas gingivalis, within atherosclerotic plaques, suggesting a direct role in their formation and progression. These bacteria can initiate or exacerbate the inflammatory processes within the arterial walls, contributing to plaque instability and ultimately, thrombotic events like heart attacks and strokes. The bacteria become “stowaways” on the bloodstream, eventually reaching and colonizing vulnerable sites far from their origin.
Oral Microbiota and Metabolic Disorders

Beyond cardiovascular health, emerging research is also shedding light on the intricate relationships between our oral bacteria and various metabolic disorders, most notably diabetes and obesity. These connections underscore the interwoven nature of our physiological systems.
Diabetes and Periodontitis: A Two-Way Street
The link between diabetes and periodontitis is well-established and bidirectional. Individuals with diabetes are at a significantly higher risk of developing severe periodontitis. High blood sugar levels create an environment conducive to the growth of periodontal pathogens and impair the immune response, making diabetic patients more susceptible to infections. Conversely, periodontitis can make it harder to control blood glucose levels in individuals with diabetes. The chronic systemic inflammation generated by periodontitis can contribute to insulin resistance, making the body less effective at utilizing insulin. This creates a vicious cycle, where each condition exacerbates the other, trapping individuals in a downward spiral of declining health. Think of it as a poorly managed building (diabetes) being further compromised by a persistent structural weakness (periodontitis), each issue making the other worse.
Obesity: Inflammation and Oral Bacteria
The relationship between obesity and periodontitis is also becoming increasingly clear. Obesity is characterized by chronic low-grade systemic inflammation, and this inflammatory state can both contribute to and be exacerbated by periodontal disease. We observe that obese individuals often exhibit distinct oral microbiome compositions, with a higher prevalence of certain pathogenic species. The inflammatory mediators released from adipose tissue (fat cells) can further fuel the inflammatory processes in the gums, creating a synergistic effect that promotes periodontal destruction. Furthermore, changes in diet associated with obesity, often rich in processed foods and sugars, can directly influence the oral microbiome, shifting it towards a more pathogenic profile.
Recent studies have highlighted the significant role of oral bacteria in overall health, linking them to various systemic conditions. For a deeper understanding of how these microorganisms can influence not just dental health but also contribute to diseases such as cardiovascular issues, you can explore this insightful article on the topic. It provides a comprehensive overview of the relationship between oral bacteria and systemic health, shedding light on the importance of maintaining good oral hygiene. To read more, visit this article.
Gut Feelings and Oral Bacteria: Beyond the Oral-Systemic Link
| Bacteria Species | Common Location | Role in Oral Health | Associated Conditions | Typical Colony Count (CFU/ml saliva) |
|---|---|---|---|---|
| Streptococcus mutans | Dental plaque | Primary contributor to tooth decay | Dental caries (cavities) | 10^6 – 10^8 |
| Porphyromonas gingivalis | Subgingival plaque | Pathogen involved in periodontal disease | Periodontitis | 10^4 – 10^6 |
| Fusobacterium nucleatum | Dental plaque and gingival crevice | Bridge species facilitating biofilm formation | Periodontal disease, halitosis | 10^5 – 10^7 |
| Actinomyces naeslundii | Dental plaque and tongue | Early colonizer, involved in plaque formation | Root caries, plaque accumulation | 10^5 – 10^7 |
| Veillonella parvula | Dental plaque and saliva | Utilizes lactic acid, may reduce acidity | Generally commensal, sometimes linked to caries | 10^6 – 10^8 |
While the gut microbiome has garnered significant attention for its profound impact on health, we are now appreciating that our oral microbiome is not an isolated entity but interacts intricately with our gut, forming a more expansive “oral-gastrointestinal axis.” This connection offers a new frontier for understanding health and disease.
Oral Bacteria as Colonizers of the Gut
It’s not uncommon for oral bacteria to travel down the digestive tract and establish residency in the gut. While many are transient, some oral pathogens, such as Porphyromonas gingivalis, have been detected in the gut microbiome and are implicated in various gastrointestinal conditions, including inflammatory bowel disease (IBD). These oral invaders, typically adapted to the oral environment, can disrupt the delicate balance of the gut microbiome, contributing to dysbiosis and potentially triggering or exacerbating intestinal inflammation. This is like a foreign species being introduced into an established ecosystem, potentially disrupting its delicate balance.
Oral Bacteria and Digestive Health
Beyond direct colonization, the chronic inflammation associated with oral diseases can also indirectly affect digestive health. Systemic inflammation initiated in the oral cavity can contribute to increased intestinal permeability, often referred to as “leaky gut.” This compromised gut barrier allows undigested food particles, toxins, and microbial products to enter the bloodstream, further fueling systemic inflammation and potentially contributing to a range of digestive and autoimmune conditions. Thus, what happens in our mouths can literally lay the groundwork for issues much further down the digestive path.
Neurodegenerative Diseases and Oral Infections
Perhaps one of the most unexpected and concerning areas of research linking oral bacteria to systemic health is their potential involvement in neurodegenerative diseases, particularly Alzheimer’s disease. This emerging field suggests that the mouth might be a backdoor to the brain.
Porphyromonas gingivalis and Alzheimer’s Disease
Recent groundbreaking research has implicated Porphyromonas gingivalis, a keystone pathogen in periodontitis, in the pathology of Alzheimer’s disease. Studies have detected this bacterium and its toxic enzymes, called gingipains, in the brains of individuals with Alzheimer’s. Gingipains are known to degrade proteins and are directly implicated in neuronal damage. We are observing that these bacterial toxins can induce inflammatory responses in the brain, contributing to neuroinflammation and potentially accelerating the formation of amyloid-beta plaques and tau tangles, the hallmark pathological features of Alzheimer’s. This suggests a potential causal link, where chronic oral infection might prime the brain for neurodegeneration. Imagine a persistent, low-grade assault on the brain, originating from what might seem like a minor infection in the mouth.
The Blood-Brain Barrier: A Compromised Defense?
The blood-brain barrier (BBB) typically acts as a highly selective filter, protecting the brain from harmful substances. However, chronic systemic inflammation, often driven by periodontal disease, can compromise the integrity of the BBB. This “leakiness” could allow bacteria, their toxins, and inflammatory mediators from the oral cavity to gain access to the brain, contributing to neuroinflammation and neurodegeneration. This is like a fortress wall developing subtle cracks, allowing enemy agents to slip through and wreak havoc within.
Moving Forward: Our Role in Oral and Systemic Health
Given the profound and far-reaching impact of oral bacteria on our overall health, it becomes unequivocally clear that maintaining excellent oral hygiene and addressing oral infections are not merely cosmetic concerns but fundamental components of holistic well-being. We have a direct agency in shaping our oral microbiome and, by extension, influencing our systemic health.
The Power of Prevention: Daily Oral Hygiene
The cornerstone of a healthy oral microbiome is consistent and effective oral hygiene. We must embrace daily brushing with fluoride toothpaste and flossing as non-negotiable routines. These practices mechanically remove plaque biofilms, disrupting bacterial communities and preventing their unchecked proliferation. Regular dental check-ups and professional cleanings are equally vital, allowing dental professionals to remove hardened plaque (calculus) and detect early signs of oral disease.
Diet: Fueling Health or Disease
Our dietary choices play a pivotal role in shaping the oral microbiome. A diet rich in fermentable carbohydrates, particularly sugars, provides a constant fuel source for acid-producing bacteria, increasing the risk of caries and dysbiosis. Conversely, a balanced diet rich in fruits, vegetables, and whole grains, and limited in processed foods, promotes a healthier oral environment. We need to be mindful of what we “feed” our oral bacteria.
Addressing Oral Infections: Timely Intervention
When oral infections like gingivitis or periodontitis occur, timely professional intervention is crucial. Scaling and root planing procedures effectively remove bacterial biofilms and calculus from below the gum line, helping to halt the progression of periodontal disease. Addressing these localized infections not only preserves our oral health but also reduces the systemic inflammatory burden and the potential for bacterial dissemination to other parts of the body.
In conclusion, our oral cavity is far more than a simple entry point for sustenance. It is a complex microbial ecosystem, a microcosm powerfully influencing the macrocosm of our entire body. Understanding the intricate relationships between oral bacteria and systemic health is not just an academic exercise; it is a call to action. By prioritizing our oral health, we are not merely preserving our teeth and gums; we are actively investing in the health of our hearts, our metabolic systems, our digestive tracts, and potentially even our brains. The evidence is mounting, and the message is clear: a healthy mouth contributes to a healthy life. We must embrace this understanding and empower ourselves with the knowledge and practices necessary to nurture our oral microbiome, transforming it from a potential source of disease into a steadfast guardian of our overall well-being.
FAQs
What are oral bacteria?
Oral bacteria are microorganisms that naturally reside in the mouth. They form a complex community on the teeth, gums, tongue, and other surfaces, playing a role in both oral health and disease.
Are all oral bacteria harmful?
No, not all oral bacteria are harmful. Many oral bacteria are beneficial and help maintain oral health by preventing the growth of harmful microbes and aiding in digestion. However, some bacteria can cause dental problems if they grow excessively.
How do oral bacteria affect dental health?
Oral bacteria contribute to the formation of dental plaque, which can lead to tooth decay (cavities) and gum disease (gingivitis and periodontitis) if not properly managed through oral hygiene.
What can be done to control harmful oral bacteria?
Maintaining good oral hygiene practices such as regular brushing, flossing, using mouthwash, and visiting the dentist can help control harmful oral bacteria and prevent dental diseases.
Can oral bacteria affect overall health?
Yes, some studies suggest that harmful oral bacteria may be linked to systemic health issues such as cardiovascular disease, diabetes, and respiratory infections, highlighting the importance of oral health for overall well-being.