A Comprehensive Guide about Gum Disease
We are all susceptible to gum disease, a silent invader that can erode the foundation of our oral health. It often creeps in undetected, a thief in the night, stealing the integrity of our gums and the bone that supports our teeth. This guide aims to equip us with the knowledge and strategies to wage a successful battle against this common affliction, from prevention to treatment.
Gum disease, also known scientifically as periodontal disease, is a spectrum of inflammatory conditions affecting the tissues surrounding and supporting our teeth. At its core, it’s a battleground where our immune system reacts to the persistent presence of harmful bacteria.
The Two Main Stages: Gingivitis and Periodontitis
We can broadly categorize gum disease into two primary stages, each with distinct characteristics and implications.
Gingivitis: The Early Warning Sign
Gingivitis represents the initial and milder form of gum disease. It is characterized by inflammation of the gums, often triggered by the accumulation of plaque. Plaque is a sticky film composed of bacteria, food debris, and saliva that constantly forms on our teeth.
What Does Gingivitis Look Like?
We might notice certain tell-tale signs when gingivitis takes hold. Our gums may appear redder than usual, losing their characteristic pink hue. They can become swollen and tender to the touch, making brushing and flossing discomforting. One of the most common and often alarming symptoms is bleeding gums, which can occur spontaneously or during oral hygiene practices.
The Culprit: Plaque and Tartar
The primary instigators of gingivitis are bacteria residing within dental plaque. If plaque is not regularly and thoroughly removed, it can calcify and harden into tartar, also known as calculus. Tartar is a rough, porous substance that acts as a magnet for more plaque, exacerbating the problem and making plaque removal more challenging. Think of tartar as a particularly stubborn stain that no amount of scrubbing can fully erase without professional intervention.
Periodontitis: The Advanced Threat
If gingivitis is left unchecked and untreated, it can progress to periodontitis, a more severe and destructive form of gum disease. This stage signifies a significant escalation of the inflammatory response, leading to irreversible damage to the supporting structures of our teeth.
The Worsening Inflammation
In periodontitis, the inflammation extends beyond the gums and into the deeper tissues, including the periodontal ligament and the alveolar bone. This is where the true danger lies, as the very support system for our teeth begins to break down.
Pockets of Infection: The Perilous Abyss
As the gums recede due to inflammation and bone loss, small pockets form between the teeth and gums. These pockets become breeding grounds for bacteria, creating an environment of chronic infection. The deeper these pockets become, the more difficult it is for us to clean them effectively, perpetuating the cycle of destruction.
Potential Consequences: Tooth Loss and Beyond
The most significant consequence of untreated periodontitis is tooth loss. The compromised bone support can no longer anchor the teeth, leading to loosening and eventual loss. However, the impact of periodontitis can extend beyond our mouths. Emerging research suggests a link between chronic gum inflammation and systemic health conditions, including heart disease, diabetes, and respiratory problems. It is a stark reminder that the health of our mouth is inextricably linked to the health of our entire body.
Gum disease, also known as periodontal disease, is a common oral health issue that can lead to serious complications if left untreated. For those looking to understand more about the causes, symptoms, and prevention of gum disease, a related article can be found at Howledge. This resource provides valuable insights into maintaining good oral hygiene and the importance of regular dental check-ups to prevent gum disease and other dental issues.
Preventing the Onset: Our First Line of Defense
The most effective strategy against gum disease is proactive prevention. By implementing diligent oral hygiene practices, we can significantly reduce our risk.
The Pillars of Oral Hygiene: Brushing and Flossing
Regular and proper brushing and flossing are the cornerstones of preventing gum disease. These daily rituals are our daily patrols, keeping the bacterial invaders at bay.
Mastering the Art of Brushing
We should aim to brush our teeth at least twice a day, using a soft-bristled toothbrush and fluoride toothpaste. The technique is crucial. We need to angle the brush at 45 degrees to our gum line, using gentle, circular or short back-and-forth strokes. We must not forget to brush all surfaces of our teeth – the outer, inner, and chewing surfaces. Neglecting any area is like leaving a crack in our defenses.
Choosing the Right Tools
The choice of toothbrush and toothpaste can make a difference. A soft brush is gentler on our gums, preventing irritation and recession. Fluoride toothpaste strengthens tooth enamel and can help combat the initial stages of decay that can sometimes accompany gum issues.
The Importance of Technique
It’s not just about the duration of brushing, but the thoroughness. We should spend at least two minutes brushing each session, ensuring we reach every nook and cranny. Overly aggressive brushing can actually damage our gums, so gentleness is key.
The Underrated Hero: Flossing
Flossing is as essential as brushing, yet often overlooked. Brushing alone cannot effectively remove plaque and food particles from between our teeth and under the gum line. Flossing acts as a precision tool, reaching into these tight spaces that our toothbrush cannot access.
Reaching the Inaccessible
We should floss at least once a day, preferably before bedtime. We need to gently slide the floss between our teeth and curve it around each tooth in a C-shape, moving it up and down to scrape away plaque from the tooth surface and just below the gum line. Neglecting flossing is akin to leaving hidden fortresses for the bacteria to inhabit.
Different Tools for Different Needs
For those who find traditional floss challenging, there are alternatives such as interdental brushes or water flossers that can effectively clean between teeth. The important thing is to find a method that works for us and incorporate it into our daily routine.
The Role of Diet and Lifestyle
Our dietary choices and overall lifestyle also play a significant role in the health of our gums.
Nourishing Our Gums: The Impact of Diet
A balanced diet rich in vitamins and minerals is crucial for maintaining healthy gum tissue. Vitamins like C and E are known for their antioxidant properties and role in tissue repair. Conversely, a diet high in sugary foods and drinks promotes bacterial growth and acid production, creating an environment conducive to gum disease.
Limiting Sugary and Acidic Foods
We should strive to limit our intake of sugary snacks, sodas, and acidic beverages, as these can feed the bacteria responsible for plaque formation and tooth decay, indirectly contributing to gum problems.
The Benefits of a Nutrient-Rich Diet
Incorporating plenty of fruits, vegetables, whole grains, and lean proteins provides the essential nutrients our bodies need to fight inflammation and maintain healthy tissues, including our gums.
Lifestyle Factors and Their Influence
Beyond diet, certain lifestyle habits can either fortify or weaken our defenses against gum disease.
The Smoking Connection: A Direct Assault
Smoking is one of the most significant risk factors for developing and worsening gum disease. The chemicals in tobacco smoke impair our immune system’s ability to fight off gum infections and reduce blood flow to the gums, making them less able to heal and more susceptible to damage. It is like pouring fuel on the fire of inflammation.
Stress and Its Consequences
Chronic stress can also negatively impact our immune system, making us more vulnerable to infections, including gum disease. Finding healthy ways to manage stress can be beneficial for our overall health, including our oral health.
Recognizing the Signs: Early Detection is Key
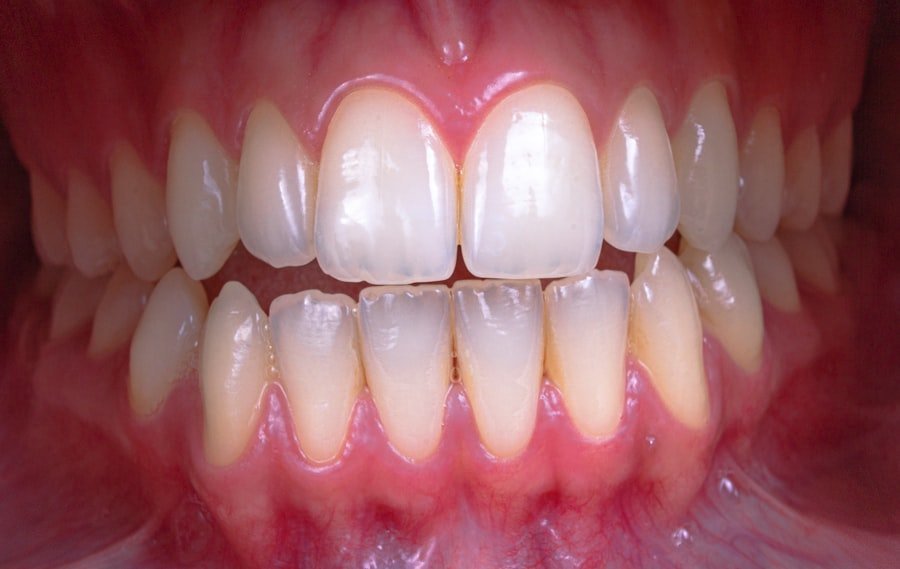
Being vigilant about the signs and symptoms of gum disease allows for early intervention, which is critical for preventing progression.
Subtle Yet Significant Indicators
Gum disease often begins with subtle changes that can be easily overlooked. However, paying attention to these early warning signs can be our early alert system.
Changes in Gum Appearance
As mentioned earlier, changes in the color and texture of our gums are important indicators. Gums that become unnaturally red, swollen, or appear to be pulling away from the teeth warrant attention.
Persistent Bad Breath (Halitosis)
While occasional bad breath can be caused by food, persistent halitosis, often described as an unpleasant, fishy, or rotten smell, can be a sign of the bacterial overgrowth associated with gum disease. This is the distinct odor of an infection brewing.
Bleeding During Oral Hygiene
Gums that bleed easily when we brush or floss are a significant red flag. This bleeding is a sign of inflammation and damage to the gum tissue.
When to Seek Professional Help
If we notice any of these signs, or if we have concerns about our gum health, it is imperative to consult a dental professional.
The Dentist’s Role in Diagnosis
Our dentist is trained to identify and diagnose gum disease. They will conduct a thorough examination, probing the gum pockets to measure their depth and assess the extent of any bone loss. They may also use dental X-rays to visualize the underlying bone structure.
Professional Cleanings: More Than Just a Polish
Regular dental cleanings are crucial for removing plaque and tartar that we cannot effectively remove at home. These cleanings are not merely cosmetic; they are a vital part of maintaining gum health and preventing disease progression.
Treatment Options: Fighting Back Against Established Disease
If gum disease has already taken hold, there are effective treatment options available to manage, halt, and sometimes even reverse the damage.
Non-Surgical Interventions: The First Line of Treatment
For mild to moderate cases of gum disease, non-surgical treatments are often sufficient.
Scaling and Root Planing: The Deep Clean
This procedure, often referred to as a “deep cleaning,” is the cornerstone of treating gingivitis and early-stage periodontitis. It involves two main steps:
Scaling: Removing the Build-Up
During scaling, our dental hygienist or dentist will meticulously remove plaque and tartar from both above and below the gum line. This is done using specialized instruments. Imagine this as clearing away the debris and fortifications that the bacteria have established.
Root Planing: Smoothing the Surfaces
Following scaling, root planing involves smoothing the surfaces of the tooth roots. This makes it more difficult for plaque to reattach and colonize, and also encourages the gums to reattach to the cleaner tooth surfaces.
Antimicrobial Rinses and Medications
In some cases, our dentist may recommend antimicrobial mouthwashes or oral medications to help control the bacterial infection and reduce inflammation. These can act as targeted weapons in our fight against the bacteria.
Surgical Interventions: For Advanced Cases
When gum disease has progressed to more advanced stages, surgical interventions may be necessary to repair damaged tissues and support.
Flap Surgery: Accessing the Problem
Flap surgery involves lifting the gum tissue away from the tooth to allow for a more thorough cleaning of the root surfaces and the removal of deep-seated infection. The gum tissue is then repositioned and sut ώστε it fits snugly around the teeth. This is like gaining strategic access to a hidden enemy stronghold.
Bone Grafting: Rebuilding the Foundation
In cases of significant bone loss, bone grafting procedures can be used to regenerate lost bone tissue. This involves placing bone graft material into the defect to stimulate new bone growth, helping to re-establish the support for our teeth. This is akin to rebuilding the walls of a crumbling fortress.
Soft Tissue Grafting: Repairing Gum Recession
Soft tissue grafting can be performed to address gum recession, where the gum tissue has pulled away from the teeth. This procedure involves taking tissue from another part of the mouth and attaching it to the area of recession, helping to protect the tooth roots and improve the aesthetics.
Gum disease is a common yet often overlooked condition that can lead to serious health issues if left untreated. Understanding its causes and prevention methods is crucial for maintaining oral health. For those interested in learning more about the implications of gum disease and how to combat it effectively, you can read a related article that provides valuable insights and tips. This resource can help you take proactive steps towards better dental hygiene and overall well-being. To explore further, visit this informative article.
Maintaining Long-Term Oral Health: A Lifelong Commitment
| Metric | Description | Typical Values/Range | Significance |
|---|---|---|---|
| Prevalence | Percentage of adults affected by gum disease | Approximately 47% of adults aged 30 and older | Indicates how common gum disease is in the population |
| Bleeding on Probing (BOP) | Percentage of sites that bleed when probed | Healthy: 20% | Marker of inflammation and active gum disease |
| Probing Pocket Depth (PPD) | Depth of gum pockets measured in millimeters | Healthy: 1-3 mm, Moderate disease: 4-5 mm, Severe disease: >6 mm | Assesses severity of gum disease |
| Clinical Attachment Loss (CAL) | Loss of connective tissue attachment measured in millimeters | 0 mm in healthy gums, >3 mm indicates periodontitis | Measures extent of tissue destruction |
| Gingival Inflammation Index | Score indicating severity of gum inflammation | 0 (no inflammation) to 3 (severe inflammation) | Helps evaluate gum health |
| Tooth Mobility | Degree of looseness of teeth | Grade 0 (normal) to Grade 3 (severe mobility) | Indicates damage to supporting structures |
| Bone Loss Percentage | Percentage of alveolar bone lost around teeth | Varies; >30% indicates advanced periodontitis | Reflects severity of periodontal destruction |
Preventing the recurrence of gum disease requires a lifelong commitment to maintaining excellent oral hygiene and attending regular dental check-ups.
The Importance of Regular Dental Visits
Consistent visits to our dentist are non-negotiable for maintaining long-term oral health. These appointments are our ongoing intelligence gathering missions.
Professional Monitoring and Intervention
Our dentist can monitor for changes in our gum health, detect early signs of recurrence, and provide timely interventions before the problem escalates. They are our trusted strategists in this ongoing battle.
Reinforcing Good Habits
These visits also provide an opportunity for our dental hygienist to reinforce proper brushing and flossing techniques and offer personalized advice for our specific needs.
Adapting Our Habits for Ongoing Success
As we age or if we have risk factors for gum disease, we may need to adapt our oral hygiene routines.
Considering Specific Oral Care Products
Our dentist may recommend specialized toothpastes, mouthwashes, or interdental cleaning devices to help us manage our individual risk factors.
Addressing Underlying Health Conditions
If we have systemic health conditions like diabetes or compromised immune systems, it is crucial to work closely with both our medical doctor and our dentist to manage these conditions effectively, as they can significantly impact gum health.
By understanding gum disease, diligently practicing preventive measures, recognizing its signs, and seeking appropriate treatment when necessary, we can take control of our oral health and preserve our smiles for a lifetime. This is not a battle we fight alone; with knowledge as our weapon and diligence as our shield, we are well-equipped to win.
FAQs
What is gum disease?
Gum disease, also known as periodontal disease, is an infection of the tissues that surround and support your teeth. It is typically caused by poor oral hygiene leading to plaque buildup on the teeth and gums.
What are the common symptoms of gum disease?
Common symptoms include red, swollen, or bleeding gums, persistent bad breath, receding gums, loose teeth, and discomfort while chewing.
How is gum disease diagnosed?
A dentist or periodontist diagnoses gum disease through a clinical examination of the gums, measuring pocket depths around teeth, and sometimes dental X-rays to check for bone loss.
Can gum disease be prevented?
Yes, gum disease can be prevented by maintaining good oral hygiene, including regular brushing and flossing, routine dental check-ups, avoiding tobacco use, and eating a balanced diet.
What treatments are available for gum disease?
Treatment depends on the severity but may include professional dental cleanings, scaling and root planning (deep cleaning), antibiotics, and in advanced cases, surgical procedures to restore supportive tissues.